How to Relieve Employee Chronic Pain (and the Associated Costs)
Employee WellnessResearch / 15 min readOur findings from our extensive research specifically around the relationships between chronic pain and comorbid anxiety and depression, and more importantly, how organizations like yours can reduce the associated downstream effects of chronic pain.
Post-pandemic life has sparked serious, record-breaking anxiety and depression levels within our workforce and the broader nation. Employees are looking to employers to offer mental health support for themselves and their families to promote sustainable and healthy lifestyles inside and outside of work. 116 million adults in the US—more than the number affected by heart disease, diabetes, and cancer combined— live with common chronic pain conditions. Of those individuals, 20-50% experience comorbid depression in parallel to their chronic pain, and are 2-3x more susceptible to suicidal ideation and behaviors.
Over the last 3 years, we’ve conducted extensive research specifically around the relationships between chronic pain and comorbid anxiety and depression, and more importantly, how organizations like yours can reduce the associated downstream effects of chronic pain including absenteeism and high medical claim costs. I hosted a webinar to discuss our findings, but here’s a recap of the discussion in case you missed it.
What is chronic pain?
Chronic pain is a long-term, debilitating health concern that affects physical, psychological, cognitive, and social functioning, resulting in downstream medical claim costs for organizations. Chronic pain conditions are associated with comorbid depression, anxiety, sleep disturbances, fatigue, neurocognitive changes, and the list goes on.
There is an estimated $560B-$635B annual total healthcare cost of chronic pain in the United States, and employee absenteeism is a well-documented cost of chronic pain.
Employees struggling with chronic pain have issues with typical day-to-day demands and activities, unable to focus on anything other than their pain, and frequently struggle with productivity and absenteeism. Individuals experiencing pain-related depression and anxiety are also likely to have worse outcomes from chronic pain. Undiagnosed and untreated chronic pain forces employees to push aside their symptoms and continue work, return to work prematurely or take sick leave stemming from stress, physical demands, and job dissatisfaction.
Drugs aren’t the answer
Opioids are known to cause bad side effects. They should be the last resort for most types of chronic pain. They can make migraines worse and more frequent and they can make lower back pain last longer. Over time, the body gets used to the effect of opioids. To get relief, patients may need to take higher and higher doses. As a result, they may become addicted to opioids. And an overdose can kill. Therefore it is generally preferable to treat chronic pain with safer methods.
Efficacy of Pain Management with AI Digital Interventions
The first study we conducted aimed to examine the differences in engagement and effectiveness of leveraging an isolated AI digital mental health intervention for users experiencing chronic pain.
Some background knowledge of the pain management study:
- There were 51 US adults with self-reported chronic pain and co-existing elevated symptoms of anxiety and/or depression that were analyzed.
- The study was over the course of an 8-week Wysa App for Chronic Pain program and acted as the only mental health resource throughout the study.
- Individuals had access to a conversational AI tool and human coaches.
The results of the pain management study
The results point to the AI digital Intervention (Wysa) as an effective, scalable solution for organizations. We found clinically meaningful improvements in pain interference, physical function, and levels of anxiety and depression.
Around the same time as our study, an independent study took place that put Wysa head to head with the usual orthopedic care and the usual orthopedic care plus in-person psychological counseling for chronic pain sufferers with symptoms of depression or anxiety. The results were outstanding. Patients who received Wysa as part of their orthopedic care reported greater average improvements in depression, pain interference, and physical function than patients who only received the usual orthopedic care. The most significant discovery was that the patients given Wysa had comparable improvements in depression, anxiety, and pain interference compared to those who received in-person psychological counseling. The app had equivalent or at par results as an in-person psychologist.
What does this mean for your organization?
Knowing that conversational AI can provide truly impactful mental healthcare to individuals struggling with chronic pain and comorbid anxiety and/or depression symptoms, AI digital interventions are the answer to scalable care, in addition to making a larger impact on absenteeism and medical claim cost savings.
Bonding with a Bot. The Importance of establishing a therapeutic alliance with digital interventions
While mental health technology is scalable and effective when used as recommended, low engagement prevents digital interventions from having their intended reach and impact. In a previous digital intervention study, participants disengaged within week 1 with average retention periods of 4-16 days. These numbers don’t evoke change.
A therapeutic alliance is one of the most robust mechanisms of change in psychotherapy interventions. Knowing that AI digital intervention has the ability to make a sizeable impact on the physical, mental, and social health of individuals who struggle with chronic pain, why do we see historically low adherence and engagement rates? The answer is simple. There is a lack of therapeutic alliance between the patient and the provider.
What is a therapeutic alliance?
A therapeutic alliance is measurable by the level of collaboration between the patient and provider on the task and goals of the course of treatment. If you don’t feel heard or understood by your provider, why would you feel inclined to return?
Establishing a therapeutic alliance with AI
If there is a lack of engagement, there will likely be low adherence to interventions and high dropout rates Top-performing health apps have an average 30-day retention rate of only 15%. People with chronic pain are 2x as likely to drop out from self-guided digital interventions when compared to traditional, guided interventions.
Two other studies which we conducted aimed to investigate how to establish a therapeutic alliance (TA) between patient and provider using AI, as well as engagement and adherence. The purpose was to examine user retention and engagement with Wysa for Chronic Pain—a digital conversational agent based on CBT principles—that is designed to improve general well-being among people with chronic pain.
Some background knowledge about the studies:
- There were 51 adults with chronic musculoskeletal pain & who endorsed coexisting symptoms of depression or anxiety (score of ≥55 for depression or anxiety) in the TA study.
- The TA study was over the course of an 8-week subscription to Wysa for Chronic Pain.
- The engagement and adherence study outcomes were user retention, defined as revisiting the app each week and on the last day of engagement, and user engagement, defined by the number of sessions the user completed.
The results of the studies: Emotional bonds with Wysa are equivalent, or even better, than human therapist relationships
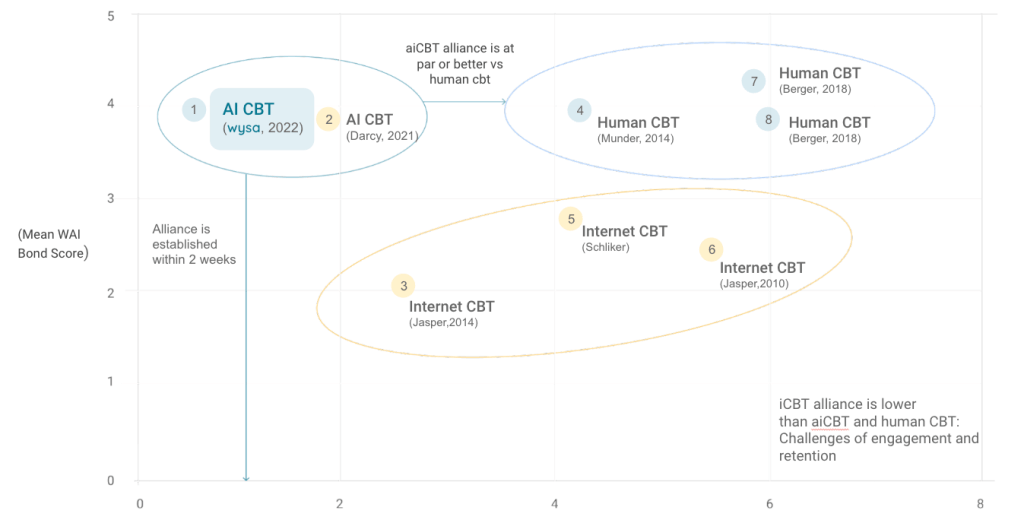
The results of the studies were enlightening. 50% of users in the Wysa digital intervention continued returning to the app each week, and the median user retention period was 51 days. High user retention and engagement, one of the biggest challenges for mental health apps today, is possible to achieve with care underpinned by digital AI by building a therapeutic alliance. High retention and engagement in your mental health solution for employees translate to a happier, healthier workforce.
Exhibit